Functional Medicine in London & Online
A client-centred, systems-based approach that explores what may be contributing to persistent symptoms – using personalised nutrition, lifestyle support and, where appropriate, functional testing.
- Book a free assessment call and we’ll match you with the right practitioner for your needs

Functional Medicine – Trained Practitioners

London Clinic & Online

Systems-Based, Practical Plans

Optional Functional Testing
Doctify reviews reflect HealthMatters Group client feedback across services
Client Feedback
“Every recommendation was linked to my symptoms and test results. It felt genuinely personalised and clear.”
– Hannah
“I finally understood what was missing and what to do next. The testing recommendation was really valuable and made the plan feel targeted.”
– Amanda
Selected feedback from NutritionalMatters clients
Book Your Free 20-minute Assessment Call
Choose a time for a free call.
We’ll listen, clarify what’s going on, and recommend the most suitable next step – including whether functional medicine is the right approach for you.
Confidential • No pressure • Clear next steps
How It Works
Step 1 — Choose a time
Book a slot for a phone call that works for you.
Step 2 — Free 20-minute assessment call
Tell us what you’re dealing with, what you’ve tried, and what you want to change.
Step 3 — Clinician match + plan
We’ll match you with the right practitioner and outline your recommended next step. If testing may be useful, we’ll explain options and costs before you decide.
Watch (1:24): What to expect from your free assessment call
Prefer to enquire first? Send us a message
FIT CHECK
Functional medicine is often a good fit when symptoms feel connected, persistent, or hard to shift with a single quick fix.
Good fit if you…
- Have ongoing symptoms and want a deeper, structured approach
- Want to explore patterns across nutrition, lifestyle, stress, sleep and environment
- Are open to a step-by-step process (with follow-ups)
- Value a personalised plan over generic advice
- Are comfortable with private fees and optional testing costs (only if recommended)
Not the right fit if you…
- Need NHS services or free support only
- Want a one-off plan with no review or accountability
- Need urgent medical care or are in immediate crisis
Safety note – If you’re unwell or at immediate risk, please contact 111/999 or your GP urgently. We’re happy to help you find the most appropriate support once you’re safe.
FEES & OPTIONS
We offer flexible time bundles so you can choose the level of support that fits your needs. After your free 20-minute assessment call, we’ll recommend the most suitable next step — with a focus on what’s likely to help, without overcommitting.
1 hour — £220
Ideal for a focused first step and clear priorities.
2 hours — £420
A popular option for an initial consult plus a follow-up to refine and troubleshoot.
3 hours — £610
For more complex goals and structured progress reviews.
4 hours — £790
Best for longer-term support across multiple priorities.
Time bundles can be used flexibly across appointments (London clinic or online).
Functional testing and supplements (if recommended) are not included – we’ll always explain options, relevance and costs before you decide.
Looking for root patterns — not quick fixes
Functional medicine takes a whole-person view: symptoms are important, but we also look for contributing factors that may be influencing how you feel. We use your history, lifestyle context and (where appropriate) testing to guide a practical plan you can implement and refine over time.
This diagram is an illustration of a systems-based approach — it isn’t a diagnosis.
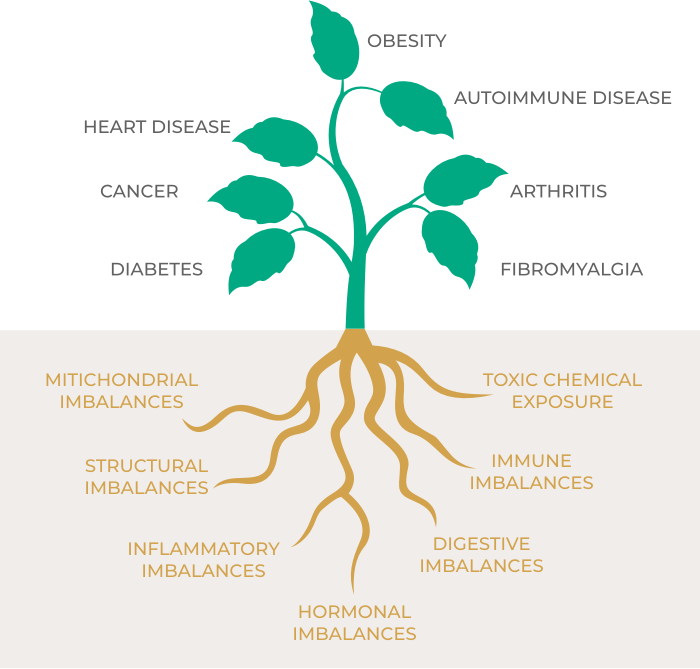
Not sure where to start? Book a free 20-minute assessment call
Areas We Help
Functional medicine can be especially helpful when symptoms are persistent, overlapping, or hard to make sense of in isolation. Here are the most common reasons people come to us:

Complex Gut Health & Digestion
Persistent bloating, IBS-type symptoms, reflux, food reactions and digestive disruption – with a structured, step-by-step approach.
Speak with our team >

Hormones, Thyroid & Women’s Health
Perimenopause/menopause, thyroid-related concerns, cycle symptoms and fertility-focused nutrition support (alongside appropriate medical care).
Speak with our team >

Metabolic Health & Weight Regulation
Blood sugar patterns, appetite/cravings, cholesterol risk factors and weight-loss resistance – focused on sustainable, evidence-informed routines.
Speak with our team >

Chronic, Multi-System Symptoms
Fatigue, brain fog, sleep disruption and “I’ve tried everything” complexity – where a systems lens can bring clarity and direction.
Speak with our team >
Also support with
Skin health • Sports performance • Cardiovascular health • Mental wellbeing
Not sure where to start? Send us a message
FUNCTIONAL TESTING OPTIONS
Functional testing isn’t always needed, but it can sometimes add clarity – especially when symptoms are persistent or complex. If we recommend testing, we’ll explain why, what it costs, how it might inform your treatment protocol, and the timeline before you decide.
Functional testing can help us explore:
- Hormone function
- Digestive function
- Thyroid function
- Nutrient status
- Food reactions/sensitivities
- Cardiometabolic markers
We work with specialist private laboratories; these tests are not typically covered by the NHS.
Functional Medicine Team & Clinical Standards
Functional medicine at NutritionalMatters is led by a single, dedicated practitioner, so you’ll receive consistent support and a clear, structured approach throughout. If your needs are complex, we can coordinate joined-up care across the wider HealthMatters Group where appropriate.
Sue Camp
Director of Clinical Nutrition, HealthMatters Group – Certified Functional Medicine Practitioner
Registered Nutritional Therapist
Special interests: Complex gut health • Hormone health • Energy, fatigue & brain fog • Metabolic health & weight regulation
What to expect: A calm, structured, systems-based approach that helps you make sense of patterns across symptoms, lifestyle and biology – with clear priorities and practical next steps you can implement and refine over time.
How We Work
- Evidence-informed, systems-based care with practical, personalised plans
- Confidential and respectful support, with clear boundaries and consent-led communication
- Optional testing: we explain why it might be useful, together with costs, before you decide
- Collaborative care where helpful (e.g., liaising with your GP/consultant with your permission)
- Appropriate onward signposting if you need a different type of support or higher level of care
- Privacy and data protection: see our Privacy Policy
We follow internal clinical governance and safeguarding standards; details are available on request.
Content owner: James Lamper, Clinical Director
Clinically reviewed by: Sue Camp, Director of Nutrition
Last reviewed: February 2026
FAQs
These answers cover what functional medicine is, what to expect, and how we use testing. If you’re ready, book a free assessment call and we’ll guide you to the right next step.
Functional medicine is a client-centred, systems-based approach that looks for contributing factors behind symptoms and supports you with personalised nutrition and lifestyle changes, and (where appropriate) targeted testing.
Conventional medicine often focuses on diagnosis and symptom management. Functional medicine focuses on understanding patterns across lifestyle, environment and physiology to inform a personalised plan – while working alongside appropriate medical care.
We review your history, symptoms, lifestyle and goals in detail, then agree on clear priorities and next steps. Follow-ups help refine the plan and track progress.
Not always. If testing could add clarity, we’ll explain why, what it costs, and what it would change before you decide
It depends on complexity. Some people want a focused plan and one review; others benefit from a short series of sessions to test, refine and build sustainable routines.
Yes, we offer both London clinic appointments and online sessions across the UK.
Still got a question?
Book a free 20-minute assessment call and we’ll point you in the right direction.
