Heart Health
- Heart Health: Protect & Strengthen Your Cardiovascular System.
- Lifestyle Support: Nutrition & Lifestyle To Optimise Cardiovascular Function.
- Tailored Programs: Invest In Long-Term Vitality & Resilience.
SUPPORTING YOU IN FINDING OPTIMAL HEART HEALTH
We are all very aware of the importance of our heart and entire cardiovascular system, but as a nation we are not doing a very successful job of having good heart health. Strokes and heart disease are responsible for about 25% of all deaths in the western world. Both conditions are referred to as ‘silent killers’ because the first symptoms or signs in many cases is a fatal event.
Heart health and cardiovascular disease is influenced by a multitude of factors, genetrics to more modifiable factors such as the foods you eat, your lifestyle as well as stress management.
If you’re concerned about your cardiovascular health, our team of heart health specialists are here to support you in creating a personalised nutrition and lifestyle plan, to keep you and your heart healthy.

MEET SUE, CLINICAL DIRECTOR & HEAD OF NUTRITION
Sue shares the benefits of working with our expert nutrition team at the HealthMatters Group
POSSIBLE SIGNS AND SYMPTOMS
The first indication that there may be a problem could be flagged in a routine screening of cholesterol or blood pressure makers with a GP.
However, if you aren’t having regular screenings or experience many of the dietary and lifestyle risk factors, heart disease can often go undetected, until a heart health crisis.
Symptoms can include
- Chest pain, chest tightness, chest pressure and chest discomfort (angina)
- Shortness of breath
- Pain, numbness, weakness or coldness in your legs or arms if the blood vessels in those parts of your body are narrowed
- Pain in the neck, jaw, throat, upper abdomen or back
Major risk factors include
- Smoking
- High blood pressure
- Diabetes
- Physical inactivity
- Prolonged stress
- Insulin resistance
- Chronic inflammation
Doctify reviews reflect HealthMatters Group client feedback across services
BOOK A CALL WITH OUR FRIENDLY ASSESSMENT TEAM
Please check Our Fees page before booking a call.
Choose a day and time that works for you.
Tell us what is going on for you.
Let us explain how we can help.
OUR FEES
Our initial 20-minute consultation is free of charge, with therapy sessions starting from as little as £120, and nutrition sessions from £200.
Packages and multi-session bundles are available – we’ll guide you to the most suitable option when we speak.
HEART HEALTH SPECIALISTS
It is hard to believe that the idea of heart disease being reversible through modifiable lifestyle choices was a radical one just 30 years ago. Today, many medical bodies emphasise the value of lifestyle interventions, and yet the encouragement of this from doctors’ offices is likely not as thorough as it could be.
When we consider the risk factors we start to understand the importance of diet and lifestyle in the management of cardiovascular health. Healthy lifestyle management signals is a powerful and necessary therapy for individuals at all points along the continuum between vibrant health, dysfunction, pre-disease and diagnosed disease. Ensuring safe and sustainable weight loss and weight management may be an important factor in keeping a healthy heart.
How our Heart Health Specialists can support you
Dietary patterns have changed dramatically in Western countries over the last 100 years. With few exceptions, studies have shown that these changes have been harmful for the populations that consume them, leading to a higher risk of nearly all chronic disease.
Our team of heart specialist nutritional therapists and dietitians will work with you to adapt your diet in a personalised way. Some of the areas they may work with include
- Saturated Fats – A review of the data has shown that diets consisting of saturated fat, trans-fatty acids, high glycemic load and low folate levels are linked to increased heart disease; while diets consisting of polyunsaturated fats, omega-3 fatty acids, low glycemic load and high in fruits and vegetables consistently lower cardiovascular risk in populations that consume them.
- Fasting Intermittent fasting has also been shown to improve cardiovascular health by decreasing oxidative stress and inflammation, improving mitochondrial function, cholesterol, triglycerides, insulin sensitivity and blood pressure.
- Micronutrients Nutrients that are essential for optimal heart health include omega fatty acids, magnesium, CoQ10, Alpha-lipoic acid, Vitamin B3, Vitamins, D, E and K and more.
We offer support from a functional perspective, and understand that statins are not the only answer to managing your heart health.

FUNCTIONAL TESTING OPTIONS
The risk of developing heart disease has traditionally been assessed by measurement of LDL-C (low-density lipoprotein cholesterol; the carrier of “bad” cholesterol) and HDL-C (high-density lipoprotein cholesterol; the carrier of “good” cholesterol).
Recent studies demonstrate that about 50% of heart attacks and strokes occur in people with ‘normal’ cholesterol levels. This suggests that many people at risk are presumed low-risk because they have “normal” or controlled cholesterol levels. Therefore, routine cholesterol tests may fail to fully identify people at risk of heart attack and stroke.
Although it is essential to assess your cholesterol levels, adverse cardiac events (such as heart attack, stroke or death) have been associated with inflammation, specifically vulnerable plaque related to increased white blood cell activation.
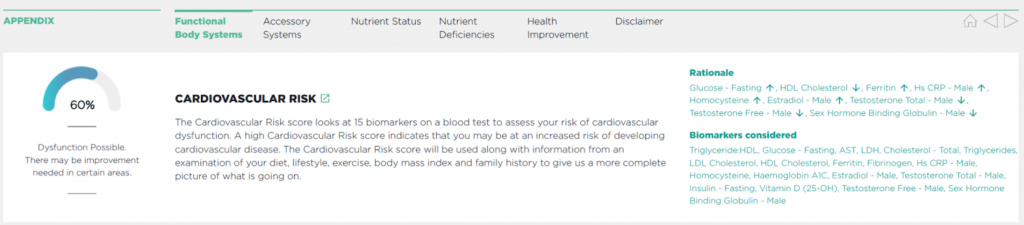
More comprehensive cardiovascular profiles including markers of inflammation such as homocysteine, myeloperoxidase, oxidised LDL and F2-Isoprostanes better help evaluate cardiovascular risk. These indicators help us understand more specifically the development of metabolic or cardiovascular disease, and the formation of vulnerable plaque which may contribute to an increased risk of an adverse event.
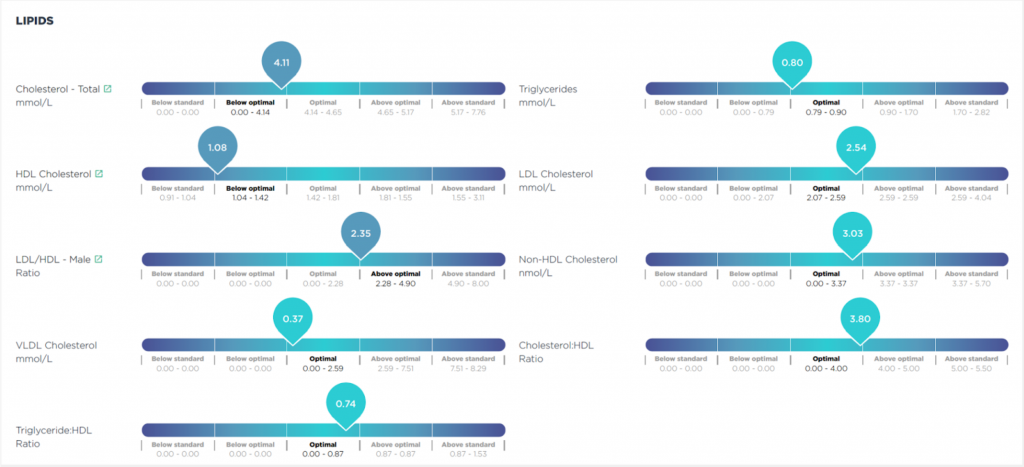
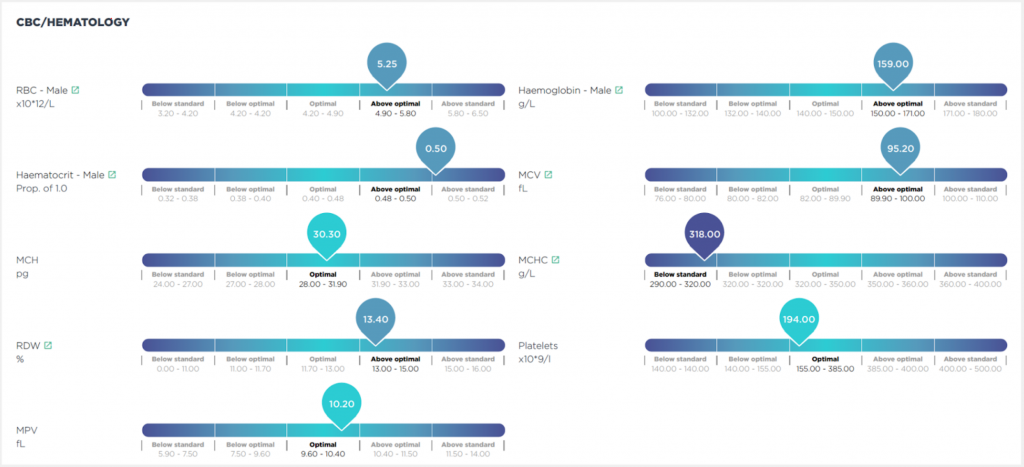
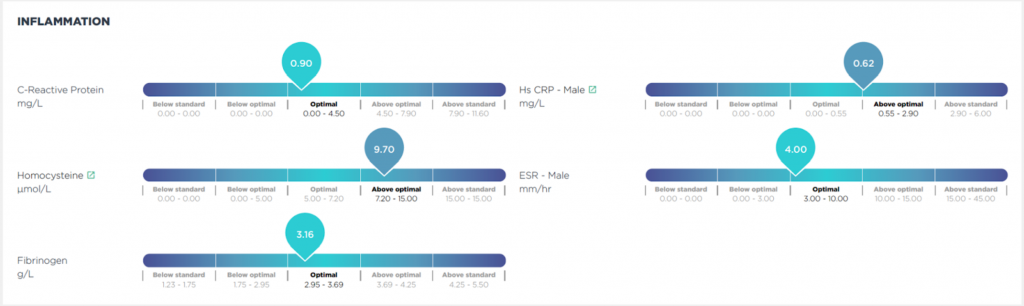
Below we have included an example of some of the markers we can test for, produced in an easy to understand report.
FAQs
What heart health issues can Nutritional Matters help with?
Common issues include conditions such as high blood pressure (hypertension), high cholesterol, and high blood glucose levels. Signs and symptoms may include shortness of breath, fatigue, and nausea or dizziness. These conditions can contribute to an increased risk for developing cardiovascular disease.
What is the role of a nutrition practitioner in supporting heart health?
Our nutritional therapists and dietitians complement medical diagnoses and GP care by identifying your unique risk factors and nutritional needs, and tailoring nutrition plans to address these. While your GP may investigate red flags or prescribe medication, nutrition support focuses on how food and lifestyle interact with your body systems. Our practitioners can work alongside your NHS GP or Consultant, as part of an integrated care model.
Can I still have support if I haven’t had a blood test with my GP?
Yes – your practitioner can work from a thorough health history and may recommend private functional testing if needed. We ask you to fill out forms prior to the initial consultation, to enable a thorough and effective nutritional analysis during the consultation.
What dietary changes will my practitioner recommend?
The science shows the benefits of dietary patterns such as the Mediterranean and DASH (Dietary Approaches to Stop Hypertension) diets. Your practitioner will put together a personalised nutrition protocol that is evidence-led, and based on a thorough assessment of your nutritional needs and health goals.
Can supplements support heart health, and will they be recommended by my practitioner?
Potentially! Supplements may be recommended as part of your personalised nutrition protocol, and will always be tailored to your nutritional needs and health goals.
What results can I expect and how quickly?
Results depend on the complexity of your presenting health or existing health condition, and commitment to making sustainable dietary and lifestyle changes. A typical timeline spans 2 – 6 months for sustained improvements, however in your initial consultation your practitioner will discuss and agree the cadence of ongoing sessions, to support the reduction of your symptoms and improvement in your health and wellbeing. Nutrition support gives you the tools to manage your health in the long-term, focusing on sustainable changes.
Will dietary changes fit with my cultural or food preferences?
Yes! Recommended dietary changes can be tailored to your preferences, in addition to addressing your nutritional needs. Practitioners adapt recommendations to align with client’s cultural diets and existing habits, focusing on modifications rather than eliminations.
How much does this cost overall?
Your first session with one of our nutrition practitioners is more than just an assessment – it’s the beginning of a relationship built on trust, expertise, and care.
Initial 60-Minute Nutrition Consultation – £200
Whether you’re managing complex symptoms or just want to feel better in your body, this is the space where your journey starts with clarity and direction.
Healing your body and transforming your relationship with food takes time.
Time Bundles give you the flexibility to shape your care around your lifestyle, pace, and needs.
After your initial consultation, you can choose to continue with a 1, 2, 3, or 4-hour bundle of time, which can be used however works best for you.
- 1-Hour Bundle – £200
- 2-Hour Bundle – £380
- 3-Hour Bundle – £555
- 4-Hour Bundle – £720
Where are we based?
The clinic is located at King Edward VII Hospital, but most services are offered remotely, making support available globally.
NEXT STEPS
We know that getting the right support starts with being truly heard. That’s why we offer a free 20-minute enquiry call – time for you to ask questions, share a bit about your story, and explore how we can support you.
During this call, a member of our experienced client support team will:
- Listen to your health goals and concerns
- Explain how our services work and what to expect
- Match you with the most suitable practitioner for your needs
This is your time – to feel heard, to feel supported, and to start moving toward the health and balance you deserve.
